|
■
Home ■ site map |
|||||||||||||||||||||||||||
|
|
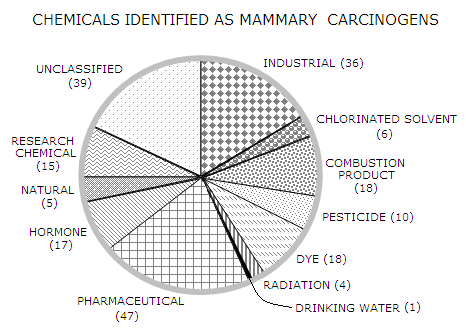
BLOG: June 2010 - December 2013 I - Breast cancer risk factors 10. Chemicals initiating breast cancerChemicals that initiate breast cancer are those capable of inducing malignant transformation either by directly damaging cell's control molecule - the DNA - or by some other mechanism. In that they are different from exogenous chemicals stimulating cellular proliferation, i.e. environmental estrogen mimics like PCBs, many pesticides (which also act as immune system suppressors), or plasticizers (phthalates), as well as from toxic chemicals that indirectly aid cancerous growth by obstructing and inhibiting body's protective functions. No carcinogenic chemical has been positively linked with breast cancer in humans. But it has much more to do with the difficulties of assessing exposures, and ethical limits of testing on humans, than with the scarcity of these chemicals, or lack of evidence that they do have such potential. Recent report has identified 216 chemicals with a record of causing or promoting breast cancer (Chemicals Causing Mammary Gland Tumors in Animals, Ruddel et al. 2007). The report is based on 450 research articles, including studies conducted by the U.S. National Toxicology Program (NTP), and those from International Agency for Research on Cancer (IARC) monographs. By the way, the report was commissioned by a non-governmental, non-profit organization (Susan G. Komen for the Cure); the zillion-dollar-question is: "What was preventing the U.S. government from creating such a report decades ago, and regularly updating it?". It hasn't been God - was it Mammon?
Some of the more familiar chemicals from each class are given in table below.
Even this short list already illustrates the extent of exposure. Paradoxically, the most numerous group of suspected breast cancer chemical carcinogens - at this moment - are among substances presumably made to support our wellbeing: pharmaceutical drugs. It is not much of a surprise when it comes to chemotherapy agents like Azacitidine, Acronycin, Adriamycin, Chlorambucil, Cyclophosphamide, Cytembena, Dacarbazine, daunomycin, Hexamethylmelamin, or Melphalan hydrochloride, even some used in breast cancer treatments (mitomycin C, thiotepa), which all act by damaging the DNA (preferably in cancerous cells). But one wouldn't (and shouldn't) expect it from diuretic antihypertensive agents (Bemitradine, Fuerosemide - the "water pill"), skin and fungal infection medication (Griseofulvin), anti-arthritic drug (Indomethacin), antibiotics (Metronidazole, Nitrofurantoin), analgestic (Phenacetin), or birth-control pill (Norlestrin). Nitroso compounds alone (within unclassified group) were found to be carcinogenic in over 90% of the 300 that were tested on animals (Gonzalez-Mancebo et al. 2004). Humans are exposed to them through food, tobacco, cosmetics, pharmaceuticals and agricultural chemicals (also, occupational exposure in rubber industry). Industrial chemicals are everywhere; benzene is in auto exhaust, plastics, rubbers, carpets, cleaners... ethylene oxide is one of the most widely used raw materials in chemical industry... nitrobenzene is used as flavoring and perfume additive... nitromethane is used as a cleaning solvent... ortho-nitrotuolene is used in production of pigments, antioxidants, agricultural and photographic chemicals... urethane (ethyl carbamate) is widely present in alcoholic beverages and fermented foods (including fermented breads and other grain products); prior to 1975 it was widely used as post-operative analgestic in Japan... vinyl chloride (chloroethane, monochloroethilene, VC, VCM), used for synthesis of polyvinyl chloride (PVC) and adhesives, outgases from electric wires and cables, plastic flooring, furnishings, toys, PVC water pipes, book covers, office supplies... similarly, vinyl fluoride polymers are used for exteriors of residential and commercial buildings, wall covers, pipes, electrical equipment, aircraft interiors... It doesn't get better with by-products of combustion. 1-nitropyrene is the primary nitrated polycyclic aromatic hydrocarbon (PAH) emitted by diesel engines. Another nitrated PAH, 2-nitrofluorene, is in the particulate emissions from diesel engines, kerosene heaters and gas burners. Yet another PAH, 2-aminoanthracene, is found in tobacco smoke and cooked foods. Benzo[a]pyrene in coal tar, car exhaust (particularly diesel engines), cigarette smoke and charbroiled foods. Isoprene is widely present natural hydrocarbon, continuously produced during metabolism and exhaled; however, isoprene as a component of (mainly) cigarette smoke has reversed flow significantly higher than natural, and can become carcinogenic. Most of the likely chemical breast carcinogens among dyes seem to be those used for hair colors (2,4-Diaminoanisole, HC Yellow no. 3), as well as those used for materials like wool, silk, lather, paper (C.I. Acid Red 114, malachite green). Many benzidine-based dyes are gradually being replaced by those with (presumably) less toxic ingredients, but its production and use are still significant. Ovarian hormones are, of course, well known breast cancer risk factor. Research chemicals are occupational hazard, of relatively small significance at the level of general population. Pesticides, herbicides and fungicides, on the other hand, can - and pretty much do - reach anybody. Some of those listed as mammary carcinogens are either banned, or no longer produced in the U.S. (captafol, chlordane, sulfallate), but it is mainly a relief for the generation now in their teens, and only partial as well. Some pesticides may persist in the environment for decades (for instance, 1,2-dibromo-3-chloropropane is still present in some well waters, more than two decades after it was banned in the U.S.), and some of those banned, or not produced in this country - such is, for instance, captafol - are still used abroad. No luck at all with atrazine, which is at present one of the most widely used herbicides in the world. Simazine is banned in the EU, but not in the U.S. 1,1-dichloroethane is chlorinated hydrocarbon with variety of industrial uses. 1,2-dichloroethane (ethylene dichloride) is mainly used in PVC production, and as degreases and paint remover. Carbon tetrachloride was widely used as a dry cleaning solvent and refrigerant; its use has declined, but remains present in the environment. Methylene chloride (dichloromethane) is a widely used solvent, used as paint stripper and degreaser, but also in food industry (for decaffeinating coffee and teas, preparing extracts and flavorings, etc.). Natural substances (including natural toxins) are not necessarily risk-free, but those with a record of being mammary carcinogens are relatively few - less than 2% of all the chemicals listed. Among them is ochratoxin A, one of the most widely spread mycotoxins (toxins produced by fungi). Any improperly stored food may be contaminated. Radiation is a major breast cancer risk factor, but it does not belong to chemicals; it is not corpuscular, rather a power (electromagnetic) field. We'd be really fortunate if our drinking water would contain only a single mammary carcinogen, out of hundreds mostly toxic chemicals contaminating it (for instance, even the very chlorine can combine with other chemical compounds present in water, forming carcinogenic compounds). But that is the state of evidence, at present. MX is only one of many water disinfection by-products, or DBP (in addition to all the chemical contaminants already present in drinking water), and it is very likely that not all of them have been identified, let alone tested. Even so, EPA estimates that 2-17% of all urinary tract cancers are due to DBPs (most of 216 chemical mammary carcinogens are mutagens, i.e. capable of causing cancer anywhere in the body). Not all of these 216 chemicals are necessarily cancerous to humans, equally toxic, or present at the levels that may influence breast cancer risk in humans. Some are no longer in use, although those that were in widespread use, and are persistent in the environment (either natural, or our living and working environment), may remain present for decades after their use has been discontinued. On the other hand, the total of chemicals tested is about 1,000 - a small fraction of over 80,000 commercial chemicals registered by the EPA. Even assuming that those tested have been to some extent preselected as more likely to be a hazard, the number of all chemicals possibly increasing breast cancer risk is certainly much higher, probably in thousands (out of 509 NTP-tested chemicals, 42, or about 8%, were found to initiate or promote mammary tumors in animals). Many of these chemicals act as endocrine disruptors, i.e. estrogen mimics; some of them are probably causing direct damage to the DNA, and others foster cancer initiation and growth through different mechanisms. Most toxins are fat-soluble, and when the body cannot effectively degrade and/or eliminate these molecules, they accumulate in fatty tissues - such as female breast. Its high rate of cellular proliferation during the adolescence, with the remnants of these immature, quickly developing cells often carried deep into adulthood, make it more vulnerable to cancer initiation and growth. Two deeply related aspects of breast cancer are its multifactorial origin, and individual variations in the mechanisms of initiation and growth. The effect of potentially carcinogenic substance is dependant on the host organism, beginning with the reaction to it by body's chemical defense - the detox system. The actual carcinogen is often produced, or "activated", after interaction of a toxic chemical with the detox system, leading to the formation of a harmful metabolite. In instances when the harmful external chemical is a direct danger, the effect will depend on how successfully it was neutralized by the detox system. Either of these two basic scenarios is determined by the interplay of a large number of factors, which is specific to every individual. The effect of substances with estrogenic activity, for instance, does not depend only on their affinity for the estrogen receptor. Depending on the cellular "context", they can produce higher or lower level of genetic response, i.e. higher or lower proliferation stimulus. It is even possible that a different cellular context turns such estrogen agonist into estrogen antagonist. In other words, a substance promoting breast cancer in some individuals may be inhibiting it in others. Another objective difficulty for identifying environmental carcinogens in our air, water, food, personal care and household products, and medications, arises from the large number of those chemicals, and the fact that many of them were present in any given time frame. Even if we'd know all the specific chemicals that are part of the exposure, it would be impossible to separate their individual effect from the effect in synergy with all the others. Obviously, not knowing which specific chemicals are breast cancer carcinogens, or may affect the disease indirectly, makes it impossible to control a study. Even more obvious, it didn't prevent those who should know better to conduct hundreds of them, without even bothering to monitor for the exposure to known carcinogens. And this uncertainty related to the role of toxic chemical exposure combines with uncertainties related to the radiation and viral exposure, as well as those arising from individual differences in chemical sensitivity. Inevitably, already very limited and often confusing research data about hundreds of possible environmental carcinogens that could be breast cancer risk factors, to what extent and under which conditions, are of little use for the individual trying to minimize its personal risk. Not only that it is impossible to avoid an invisible enemy, in minimizing breast cancer risk it is often impossible to avoid it when in full sight. Simply put, we are immersed in the sea of toxic chemicals, and there is no way out of it. Minimizing the exposure is only one part of the equation; the other is taking care of one's "cellular context", i.e. doing the best to give to your cells nutrients they need to protect and promote their proper function. YOUR BODY ┆ HEALTH RECIPE ┆ NUTRITION ┆ TOXINS ┆ SYMPTOMS |