|
■
Home ■ site map |
|
|
BLOG: June 2010 - December 2013 I - Breast cancer risk factors 7. Factors predisposing for breast cancer: Toxins...In addition to diet, the other major breast cancer (BC) predisposing factors that can be influenced by a woman are: 1. those related to the body's toxic exposure, 2. body's immune-function, and 3. multitude of lifestyle-related factors, most of which to a greater or lesser degree also affect the previous two. With breast cancer - and with degenerative diseases in general - multiple factors, including those seemingly unrelated, are part of the same complex mechanism that makes the body vulnerable. They overlap in their action, and often reinforce each other. Addressing all known factors, as opposed to focusing on a single factor, or a limited set of them, may make a difference between preventing a disease, or not. The more we know about predisposing risk factors, the better chances to stay healthy. This is why it is important to be aware of all the potential risk factors, and then weight their actual importance according to the individual situation. 1. Toxic overload The efficiency of body's detox function and the effect of accumulated toxins on cellular health is probably the most neglected factor in the area of cancer research and treatment in general. Breast cancer research and treatments are not the exception. A few U.S. studies investigating the link between one of many omni-present environmental toxins, pesticides, and breast cancer, did not find positive correlation. If they did, it would hardly mean anything as well, since the studies not only lacked reliable method of assessing actual exposures, particularly at the time when it matters most, during the adolescence, but didn't even try to assess individual levels of vulnerability to that type of toxic exposure among the study population. Needless to say, leaving this vital factor uncontrolled makes proper randomization impossible, and makes any results meaningless. Knowing that the detox system efficiency, and vulnerability to toxins can vary individually up to a hundredfold, or more, makes such studies laughable, if they wouldn't be just plain sad. What matters at least as much as the nominal exposure to toxins is body's ability - or inability - to neutralize them. Real body exposure is the one occurring inside, after the detoxification process. And then much depends on body's repair efficiency, which also varies widely individually. If study participants are not properly randomized with respect to these crucial risk factors - and no one does this kind of randomization - any result from such a "study" is entirely meaningless. Knowing that nutritional status of the participants is never controlled (i.e. known) factor in these studies does not make the picture any better. Nor is the exposure to other carcinogens and toxic substances. Or exposure to stress, viral carcinogens, And so on. Some real-life data, such as substantial reduction in breast cancer incidence in Israel, after it banned many toxic chemicals in 1978, support this very logical association between toxic chemicals and breast cancer (the ban was triggered by an Israeli study that did find link between toxic chemicals and breast cancer). Breast cancer incidence in Israel dropped despite all other recognized risk factors worsening in the Israeli population, and despite continuing rise in the world breast cancer mortality rates. Of course, pesticides are only the tip of the iceberg; many other known and unknown potential carcinogens are present in our water, food and living environment. Many toxins that are not directly carcinogenic do have the ability to interfere with body functions at all levels, possibly becoming a piece of the puzzle in the initiation and growth of breast cancer. Others, like chlorine - yes, chlorine from chlorinated water too - can form carcinogenic compounds combining with other not directly carcinogenic compounds and metabolites. Very little research is done in this direction, and much of what has been done is incompetent. And no research whatsoever has been done on the aggregate effect of all carcinogenic and non-carcinogenic toxic chemicals and their metabolites in human body combined. There are anywhere from hundreds to thousands of
such chemicals circulating child or adult. And toxic overload of chemicals that inhibit body functions and do direct damage to it - separately from carcinogenic chemicals that have potential of initiating malignant cell transformation - is not only predisposing for breast cancer, it is all but certain to be stimulating its growth as well. Is it wonder that we remain in dark when it comes to the causes and treatment of cancer? 2. Suppressed immune-response In addition to body's detox system, efficient immune-system is a must for breast - and any other - cancer prevention or cure. While the detox system protects the cell from damage - structural or functional, or both - by toxic substances in general that can lead to malignant transformation, the immune system protects the body by destroying deviant cells and - in the context of predisposing breast cancer factors - by preventing viruses from actively infecting the body. There is a good bit of evidence suggesting that viruses can play an active role in the initiation and progression of most cancers - including breast cancer. It is not unthinkable that their activity could also predispose - i.e. make the body more vulnerable - to breast cancer. As complex as the immune-system is, it is inevitably affected by many factors, beginning with one's diet. Not only that it depends on diet for getting the nutrients it needs to function properly, it can and does get negatively affected by some common foods, or by metabolic deviations resulting from poor diet. Specifically, whole food diet with plentiful plant foods - particularly green leafy vegetables - supports the immune function. On the opposite end, the common combination of sedentary lifestyle and poor food choices of excess animal and processed foods raises body lipids - cholesterol, free fatty acids, triglycerides - and they in turn inhibit proliferation, mobility and killing efficiency of white blood cells. Another poor diet staple, sugar - in any form: sucrose, fructose, honey - directly inhibits white blood cell activity for hours, starting within half an hour from ingestion. The more sugar consumed, the more suppressed immune system. It is unclear how, specifically, it works, but it is probably related to the elevated blood glucose level, and the dependency of nutrients stimulating white cell activity on cross-membrane transport by insulin. Since unloading glucose from the bloodstream is body's priority, such nutrients - for instance, vitamin C - and other compounds needed for the cellular process get shortchanged by glucose in their access to the cell. In addition to diet-related immuno-response factors, the immune system function is adversely affected by a multitude of other factors, from the presence of chronic hidden internal infections, to high stress levels, and even to negative emotions, grief and sadness. It shows how everything in the body is inter-connected and inter-dependent. Chronic hidden internal infections There are numerous forms of chronic internal infections that can overburden and weaken the immune system. Among the most common are probably infections inside the mouth (teeth/gums/jaw), such as cavities, toxic and immunologically incompatible fillings, or infected root canals. Such infections lower immune efficiency and, particularly when combined with other risk factors, can make cancerous growth possible. And, if they are part of it, such hidden, unaddressed factors can obstruct any therapeutic attempt, and prevent recovery, as long as they remain unresolved.
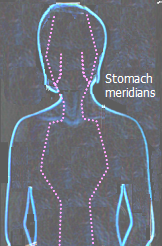
energy meridians (which are positively proven to exist). Having, for instance, infected teeth (that includes root canals, which very often harbor hidden infection), or metal implant on either side of the jaw, can interrupt energy flow along the acupuncture meridians passing through the breasts (specifically, stomach meridians, illustrated at left). It can compromise integrity of the cellular processes in the breast tissue, contributing to the development of breast cancer. Goldberg's "Definitive guide to cancer" (p600) cites a Swiss clinic director, doctor Thomas Rau M.D., stating that about 90% of breast cancer patients at his clinic had dental factor involved, with possible negative effects on both, energy meridians and immune efficiency. That by itself means little, without knowing the incidence of the same affliction in a comparable healthy population. But the fact that a qualified medical professional points out to it indicates that, in his experience, it could be a significant factor It is mentioned above that overgrowth of intestinal yeast could lessen body's resistance to breast cancer. That can be expanded to all toxic microorganisms residing in the intestinal tract. Century ago, much less processed foods eaten back then would pass the intestine in less than 24 hours. These days, 2-3 times as long is common. The longer food stays inside, the more rotting, more bad bacteria, more toxins. Many have chronically elevated intestinal toxicity, which does not cause apparent (i.e. clearly related to it) symptoms, but does cause, or lead to the scores of "unexplained" symptoms and, slowly - or not - ruins one's health. Also, remember, 50%, or so, of the entire immune system army is committed to the intestinal tract. If there is one part of the body that, if compromised, drains and weakens the immune system, it is your intestines. Unfortunately, chronic hidden internal infections belong to the long list of breast cancer risk factors ignored by the official medicine. Psychological drain Prolonged or excessive mental stress and emotional distress negatively affect the body in many ways. We are all exposed to it at work, in our family and other social environments, even alone. Actual stress level is a function of two main variables, stress exposure and personal susceptibility. Given exposure, the most significant factor in creating stress level is either personal level of fear, from feeling threatened by a possible negative outcome (realistic, or not,, mainly dictated by one's self-image), or anxiety from difficulty to meet excessive demands imposed onto oneself by others or oneself. Either way, prolonged stress has profound effect on the body function. In general, stress stimulates cardio-respiratory function, while suppressing body's metabolic, regulatory and protective functions, including the immune system function. Needless to say, chronically suppressed metabolism, and with it body's metabolic lifeline and regeneration, inevitably undermines health and invites disease. More so with the stress hormones inhibiting activity of white blood cells and suppressing their production, literally making the thymus gland shrink. Obviously, that increases vulnerability to cancer. A study from 1990s found that women who had significant emotional trauma within 6 years before being diagnosed with breast cancer had 5 times higher incidence of the disease (Trichopoulos et al. 1996). How you treat your emotions may matter just as much. Research results consistently show that personality type that suppresses emotions is much more likely to develop breast cancer than free-personality types, habitually letting them out. It is probably not the suppression of emotions itself that does most of the damage - rather the reason behind it. The only reason not to act naturally is some form of perceived threat if one does; in other words, such personality is in the state of nearly constant stress/anxiety. And that takes its toll. Two worst offenders are holding inside "negative" emotions, such as dissatisfaction or anger, and hopelessness - a byproduct of either extraordinary difficult circumstances or, much more often, the negative self-image. Those are not inherent forms of behavior, rather acquired in the process of growing up. Hence, they can be positively influenced - which does require resolve and will - and modified into more natural, healthier, and happier behavior. In contrast to behavior dictated by a constant anxiety state, such inner environment promotes - or should we say allows - optimum body functioning. And that feels down to a single body cell. 3. Lifestyle risk factors Put simply, healthy lifestyle requires just four things: eat well, stay clear of toxins/carcinogens, move your body around, and let yourself be happy - there is always a good reason for it. Eating well means eating foods close to their natural state. The closer, the better. Just make sure they have no toxic "extra". Stay clear of toxins because they are, well - toxic. Move your body around because it's been made for it. Once you stop, it becomes - well - kind of rusty. And you know what happens to rusty things. They rust more, and fall apart. Be happy, because your body knows when you're not. How does it know? By taking from its metabolic/regenerative functions, it makes it unhappy too. That was a bit different take on the worn out theme of "healthy lifestyle". And, really, most often we do know what is the right thing to do, and what is not. We shouldn't eat nutrient-depleted, toxin-laden foods. Shouldn't become excessively overweight. Let stress take over our lives. Think negative. Smoke. Drink. Why not? Because any of it - and combined more, or much more so - weakens the body, making it the easier pray for a disease. Including breast cancer. Let's take, for instance, alcohol. Alcohol consumption Research on the link between alcohol consumption and breast cancer is sparse, but what is there is very alarming. As little as 2-3 alcoholic drinks *a week* could increase breast cancer risk up to 2-3 times (Schatzkin et al. 1987, Willet et al. 1987, Longnecker et al. 1988); while this is probably too pessimistic, it seems quite possible that even moderate regular consumption of alcohol can significantly increase the risk of getting breast cancer. Multiple studies were consistent in finding that the breast cancer risk increase due to alcohol consumption can be approximated with 10% risk increase with every 10g of alcohol consumed daily, for longer periods of time (Smith-Warner et al. 1998, Hamajima et al. 2002, and others). This held independently for beer, wine and liquor, so it is safe to assume that alcohol in any form of consumption will have similar effect. Specific mechanisms through which alcohol promotes breast cancer are not yet determined, but should be at least in part related to its effects on depleting nutrients, particularly vitamin B9, as well as to inducing oxidative damage and burdening detox system. These days, many of us have detox system overwhelmed by constant exposures to hundreds of toxic pollutants. If, for instance, aldehyde pathway - which is the route for detoxifying alcohol - is clogged by high toxic exposure and/or nutritional deficiencies lowering its efficiency, alcohol consumption may disrupt normal detoxication process, resulting in the formation of very toxic metabolites. Primary metabolites of alcohol, aldehydes, are already more, or much more toxic than alcohol itself (it is mainly their effect that causes hangover symptoms), and if not neutralized during continued detoxication process, it can trigger formation of real nasty metabolites, forming damaging stable bonds with body molecules (adducts). Clogged aldehyde pathway can also result in formation of epoxides, another form of potentially very toxic metabolites, which can be carcinogenic. In individuals with marginal detox/antioxidant efficiency and/or increased vulnerability, these toxic metabolites could cause more significant and possibly irreparable damage to the cellular structures, including DNA. Some studies do indicate that acetaldehyde, primary metabolite of alcohol, may have mutagenic effect (Garro et al. 1990, Castro et al. 2006). This toxic compound is also produced by Candida albicans intestinal yeast, so fungal overgrowth may also, under certain circumstances, become a breast cancer risk factor. Consuming alcohol suppresses the immune system by impairing white cell mobility. Alcohol could be also contributing to elevated plasma level of estrogens (Hankinson et al. 1995). That is probably not all, but is already more than enough. Keep in mind that breast cancer is always a complex disease, with a number of negative factors combining to form the environment allowing breast cancer to grow. What we know about alcohol and its biological effect clearly puts it among those negative factors. This rounds up this overview of factors predisposing for breast cancer. Following page turns toward the crucial moment in breast cancer genealogy: factors that actually initiate cancerous transformation in the breast YOUR BODY ┆ HEALTH RECIPE ┆ NUTRITION ┆ TOXINS ┆ SYMPTOMS |
 But
such infections may affect negatively body functions other than the
immune system as well. Somewhat unusual, but
very realistic negative aspect of such infections is their effect on
body's
But
such infections may affect negatively body functions other than the
immune system as well. Somewhat unusual, but
very realistic negative aspect of such infections is their effect on
body's