|
■
Home ■ site map |
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
BLOG: May 2010 Hypertension risk: time to move beyond salt?
Salt war -
Salt
hypothesis -
Dahl/Intersalt -
Salt
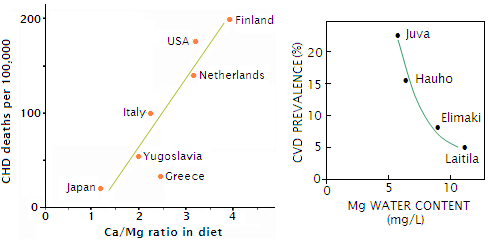
studies The purpose of the entire recent move to reduce salt intake at the level of population is hopeful - but unsupported by the facts - expectation of significantly reduced rate of hypertension, and related adverse health effects. Is there something in the body of evidence suggesting better options? There sure is. And it is not a secret. In a blitz, if the goal is to curb hypertension by a concentrated effort of the officials and food manufacturers, then: ▶ reduce caloric value of processed foods, with particular attention paid to their glycemic index, and ▶ increase their nutritional value, particularly their potassium and magnesium content Other processed food aspects can be addressed as well, but these two are of major importance. In addition, promoting specific aspects of a healthy lifestyle, such as consumption of fruit and vegetables, regular physical activity, minimizing alcohol consumption and further reducing rates of smoking, would benefit health of the population in general. In particular, it would help reduce raising rates of hypertension, and further reduce the rates of cardiovascular diseases (CVD). The above two processed food interventions are at least as doable as reducing its salt content - chances are, more so. Unlike reducing salt intake, their positive effect on promoting cardiovascular health is consistent and undisputable in the existing evidence. Furthermore, added potassium and magnesium would little affect food taste, which would make it much easier on food industry to implement. Then - why not? Is it possible that no one among the interventionists even mentions this undoubtedly superior option because it doesn't play to to the hand of salt doctrine, that is, does not reaffirm the existing salt policy or, in a broader aspect, the conventional cardiovascular disease risk factors? I'd say it is more than possible - it is very likely. At best, the heart-friendly mineral option may get to be used as a near-anonymous addition to the set of "proven" remedies - reduction in saturated fats, cholesterol and salt intake - as it's been done in Finland, by ensuring widespread use of the special reduced-sodium, magnesium/potassium-enriched salt (Mineral SaltR, Salvo-Companies, Helsinki). This is despite the importance of minerals for cardiovascular health being well known for quite a while. As far back as 1970s the evidence was clearly indicating that minerals do play important role in cardiovascular health. Good, bad or ugly. As the Finnish CVD project, hopeful of healing the heart of the nation, was expanding, a detailed assessment of Finland's regional water and soil mineral contents was done (Minerals, Coronary Heart Disease and Sudden Coronary Death, Karppanen et al, 1978). It showed significant differences in soil/water contents of magnesium. Also, that CVD mortality rates throughout Finland are in inverse relation to it (and inversely with the mineral content of water in general). North Karelia, with the highest mortality rate had also the lowest soil/water magnesium level, nearly 2.7 times lower than in the region with lowest mortality rate (122 vs. 324 mg/L of arable soil). Widening the focus to other countries brought in an intriguing relation between CHD mortality and dietary calcium-to-magnesium ratio. As the plot shows, the mortality rate rose sharply with the ratio.
Plot to the right shows correlation between prevalence of cardiovascular disease (CVD) and drinking water's magnesium content in four Finland localities (300 men aged 24-70y, Luoma et al, 1973). For coronary (ischemic) heart disease, the correlation was even stronger: 8.6% vs. 1.1% (worth mentioning is that the average blood cholesterol level was only 5% higher in the high CVD prevalence region). Sure, we've seen plots like these before, and know very well that such dramatic statistical correlation can mean little, or nothing at all. But since two major essential minerals are involved, it calls for a closer look. Needed for activation of more cellular enzymes than any other mineral, magnesium is vital for proper muscular function in general, and for the cardiac function in particular: sodium/potassium channels functioning, signal transmission, mitochondrial and many other functions and processes within myocardial cells. Magnesium-depleted heart muscle becomes prone to arrhythmias, tissue damage, myocardial infraction and sudden cardiac death. Sudden coronary death accounts for over 300,000 U.S. deaths annually. Does it indicate generally insufficient magnesium levels as a possible factor? You bet. Populations in soft water (i.e. low in minerals) have lower level of magnesium in their heart muscle and arteries than those in hard water (mineral-rich) regions. CHD patients routinely have lower magnesium levels than healthy individuals. Low myocardial magnesium content is typical in sudden death from heart disease, and so on... All right, but what the dietary calcium-to-magnesium ratio has to do with CVD mortality? It is probably the indication of low magnesium intake that matters more here, but excessive calcium can be harmful as well - the lower magnesium, the more so. Alteration of intracellular calcium balance is an inseparable part of hypertension (and, for that matter, cardiovascular disease in general). And it is directly related - among other factors - to the sodium channel function, which depends on sufficient magnesium levels. Low magnesium inhibits the ion channels, causing loss of cellular potassium, and increase in sodium; this in turn can cause influx of calcium into the cells, and with it increased contractility of the heart muscle and arterial walls. High calcium levels could intensify this effect. Also - under certain unfavorable circumstances - calcium can and often does promote atherosclerotic process; in addition it inhibits absorption of magnesium, and can also accelerate its loss. In fact, just a little closer look at what is taking place in the heart muscle clearly shows that it is not about any single element. Prevalence of heart diseases and related mortality has strong positive correlation to a product of the Ca/Mg and Na/K ratios. The larger it is, the higher CVD morbidity and mortality are likely. That doesn't make neither calcium nor salt "bad": what is bad is mineral imbalance. We don't need to fear deficiency of either calcium or sodium. However, the situation with the other two minerals is much less safe. Magnesium deficiency is rather common in developed countries. On top of steadily decreasing intake due to soil depletion and loses in food processing, magnesium levels are further suppressed by (in addition to already mentioned calcium) high intake of a number of nutrients, including sodium, potassium, vitamin D and copper. Body magnesium level is also lowered by high-glycemic diet (due to the higher insulin level), high alcohol consumption, or smoking. Smoking affect heart by reducing its oxygen supply, which not only diminishes energy available to the heart muscle, but also causes loss of magnesium from its tissue. In addition, cigarette smoke contains cadmium, a nephrotoxic, cardiotoxic mineral ("heavy metal") causing damage to the kidneys, heart and blood vessels. It is commonly found in high levels in the urine and kidneys of hypertensive patients. Regional variations in exposure to cadmium relate directly to the corresponding rates of cardiovascular diseases. And there's more trouble for magnesium - and the heart - in store. High levels of catecholamines (stress hormones like adrenaline, noradrenaline and dopamine) can cause myocardial damage by instigating a combination of magnesium loss and calcium overload, accompanied by a drop in energy production of the myocardial cells. This little digression to a few minerals other than sodium, and their role in cardiovascular health, leads to quite a different - and, chances are, more factual - interpretation of Finland's CVD problem, and likely reasons behind its turn for the better. The Fins confronted what they thought were the culprits: high fat intake - particularly saturated fat intake from dairy products they thought causes high cholesterol - high blood pressure and high rates of smoking among Finnish men. Cutting down on saturated fats may have helped, but almost certainly not as much as increased intake of good fats that we need. Cutting down on dairy had moderated high calcium intake
and helped
which, with increased intake of this mineral deficient in Finnish diet (according to Karppanen, the average 24 hour urine magnesium excretion in Finland was around 125mg, indicating significantly lower intake than present estimates of over 400mg/day), correcting Finland's excessively high Ca/Mg ratio. Likewise, reduction in salt intake lowered Finland's Na/K ratio. Note that does not imply that the nominal salt intake in Finland was excessive: rather than it was excessive relative to low intakes of potassium and magnesium. Probably the most significant single factor in reducing CVD mortality in Finland was large reduction in the incidence of smoking among men, from 45% in 1972 to 28% (incidence of smoking among Finnish women had slow raising trend during most of this period, but it is still only 18%). The downtrend in hypertension and CVD mortality rates was certainly helped by the improved balance between four major minerals, magnesium, calcium, potassium and sodium, as well as by better treatment efficacy and nutritionally superior diet, particularly higher intake of cardio-protective antioxidants and fatty acids. Lower saturated fat intake, by itself, or somewhat lower cholesterol level, probably had only marginal effect. This brief summary is far from being all-inclusive; there is a number of other factors that, either alone or combined with others, can significantly affect CVD mortality and morbidity at the level of population. It merely introduces one such significant factor: body level of the four major body minerals, and the consequences of their imbalance. While the above plots for calcium and magnesium are almost certainly statistical distortion - possibly significant - of the actual association strength, it is a scientific fact that these two minerals, as well as potassium, sodium, and score of others, are vital to body function and cardiovascular health. To illustrate this, we don't have to move away from salt. After century-long investigations, it is not even certain that the "active ingredient" in salt affecting blood pressure is sodium. Initially, researchers believed it is chloride, but the opinion that it is, in fact, sodium later prevailed. However, the evidence directly questions this widely accepted view. As far back as 1929, Berghoff et all reported that high sodium level raised blood in hypertensive patients when consumed as sodium-chloride (salt), but not when consumed as sodium bicarbonate. More recent investigations found that replacing sodium-chloride with sodium bicarbonate actually lowers blood pressure, in both hypertensive and normotensive individuals (Luft et al. 1990, Schorr et al. 1996). Sodium has no effect on blood pressure when combined with other anions, as well (sodium phosphate, sodium citrate, Boegehold et al. 1991). Similarly, reduction in blood pressure of hypertensive patients following potassium intake is markedly lower with potassium chloride than with potassium citrate. Luis Dahl would have scratched his head in disbelief had he administered sodium bicarbonate, instead of salt, to his salt-sensitive strain of rats: despite identical high plasma levels of dreaded sodium, there was no hypertension (Whitescarver et al. 1984). Note that Dahl did test the effect of chloride alone, and did not find that it raises blood pressure in rats; that, however, is contradicted by recent research (Schmidlin et al. 2005). The point is that the CVD/hypertension problem is far too complex to
be dealt with effectively by a simple More so considering that the existing evidence does not support the notion that sodium plays significant role in it at the level of population. Sodium can be significant hypertension factors for individuals, those far exceeding average intake level and for vulnerable sub-populations, but its importance in this respect pales in comparison to a number of other factors. Let's take a look.
Any of the above factors - and some others - can be significant, or not, in any given case of hypertension. And so can interaction of any number of these factors (note that the above list of effects are limited to some of those most relevant, and a gross oversimplification of all possible effects that any of these factors can produce, alone or combined). The two immediately apparent implications are: (1) hypertension is a complex disorder, potentially involving a number of factors, and (2) studies not controlling all possibly significant factors - and not one study so far even came close - will give incomplete, unreliable, possibly misleading or contradicting results It is also obvious how disproportionate to its actual role is the attention given to salt (sodium) alone. Coupling it with the lack of evidence of it being significant hypertension factor at the level of population, it becomes even more puzzling what is it that earned to salt reduction schemes such a firm official support. Part of the answer, as mentioned before, is the attempt to confirm decades long official policy on salt, despite overwhelmingly unfavorable research results. But there could be more to it: a silent, invisible but powerful backing to these recent population-wide salt reduction initiatives. Let's face it - the sick are a big business these days. Directing attention, energy and funds into something that will have little, if any effect on actually making people healthier - as opposed to meaningful, diet-lifestyle-environment based alternatives - is nearly as good for that business as keeping the status quo. Don't think this business hasn't realized that, and taken the appropriate side. So, the fact that, for instance, pharmaceutical companies are lining up behind organizations promoting salt hypothesis and/or salt reduction programs shouldn't be much of a surprise. This informal alliance of policy makers and mighty, influential "interested party" profiting on the sick is probably the back bone of the salt hypothesis resiliency in face of the mountain of unfriendly research data, as well as the prime force behind salt-reduction initiatives. Can this fact-deprived salt reduction scheme succeed? It might, since most of people won't go through the mountains of research data, and will simply pick the side to believe to. For most, it will be the official view. Before spending weeks on getting the actual facts, I believed it too. I even cut down somewhat on my (moderate) use of salt, "just in case". After becoming familiar with research record, I know that
quality of a diet and lifestyle is much more important
than As for making salt intake reduction part of the public health policy, it needs to answer two simple questions: 1 - Is it the best way of achieving desired goal, and 2 - Is it safe? The answers are just as plain and simple: no, it is not the best way, and we don't know if it is safe. Salt intake reduction, even if accomplished as planned - and that is a big "if" - doesn't even come close to all the benefits of a healthful diet and lifestyle. That cannot be overemphasized, and shouldn't have been sidetracked in the salt intake reduction programs promotion. Based on available evidence, even magnesium and potassium alone, added to processed foods, would be more effective and safer alternative. Talking about the big "if", there is a serious discrepancy between FSA (Food Standards Agency, U.K.) claims of 9.5% reduction in the population salt intake, based on the reduction in processed foods salt content, and direct measurements in 13 public surveys (the last being the National Diet and Nutrition Survey in 2008, more details in Can Dietary Sodium Intake Be Modified by Public Policy?, McCarron et al, 2009), indicating no appreciable change in U.K. sodium consumption. Any takers? Seems that the U.K. population has found the way to compensate for salt taken away by its clever health bureaucrats. And that may have been for the better: the fact is that we still know so little about the role of salt in the body, in general and more so individually, that any attempt to externally modify its intake for the entire population amounts to a reckless adventure. That only adds to the advantages of the alternative: making processed foods more nutritious, as mentioned at the top, particularly with respect to magnesium and potassium. Such limited-scope public health policy would be safe, and certainly more effective than attempts on sodium intake reduction. Between knowing that salt intake reduction at the level of population nearly certainly won't work in lowering hypertension rates and CVD toll, and not knowing how safe it is, there is not much going for this officially touted "solution". YOUR BODY ┆ HEALTH RECIPE ┆ NUTRITION ┆ TOXINS ┆ SYMPTOMS |
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
No one has commented yet. Be the first!